Surgery
The morning of surgery is when I go under the knife again for Baclofen pump No. four. I wake early to the sounds of a busy ward. Trollies are clattering, and wheels are squeaking as they pass my door. A hubbub of voices with different accents converses with each other. It isn’t easy to make out what they are saying.
I haven’t eaten since teatime yesterday, which was only a couple of sandwiches. I hope I am first on the list to go to the theatre for surgery.
A lovely nurse pops in to take my Obs. My blood pressure (BP) is as expected, heart rate OK and temperature steady 36 point something. The nurse doesn’t know when I’ll be going down.
For surgery, a general or not?
After a while, the same morning of my surgery, about 11 am, the anaesthetist came in to discuss my anaesthetic. His name is Mo. We have met before in my pre-op assessment. He seems cool, and I have confidence in his skill of keeping me alive.
If I opt for a spinal block, I will be awake during the procedure. Using a general anaesthetic is more comfortable. I pause, thinking for a moment, could I handle being conscious during the theatre time? I decide to go completely under. He confirms that is a good option and leaves.
I get the opportunity for a shower before the afternoon procedure and wish I hadn’t bothered. I know the water supply for the hospital must be in demand. However, the ridiculous stream of aqua coming from the showerhead is quite disappointing. It might be OK compared to other shower facilities, but compared to what I’m familiar with at home! But still, it was refreshing.
Time to go for surgery
The chance for surgery in the morning has passed, and the afternoon arrives. A porter appears to accompany me to the pre-operative room where the action starts. Leaving my room, I travel down the corridor to the lifts. Down another couple of passages and arrive ready to go under the knife.
Under I go
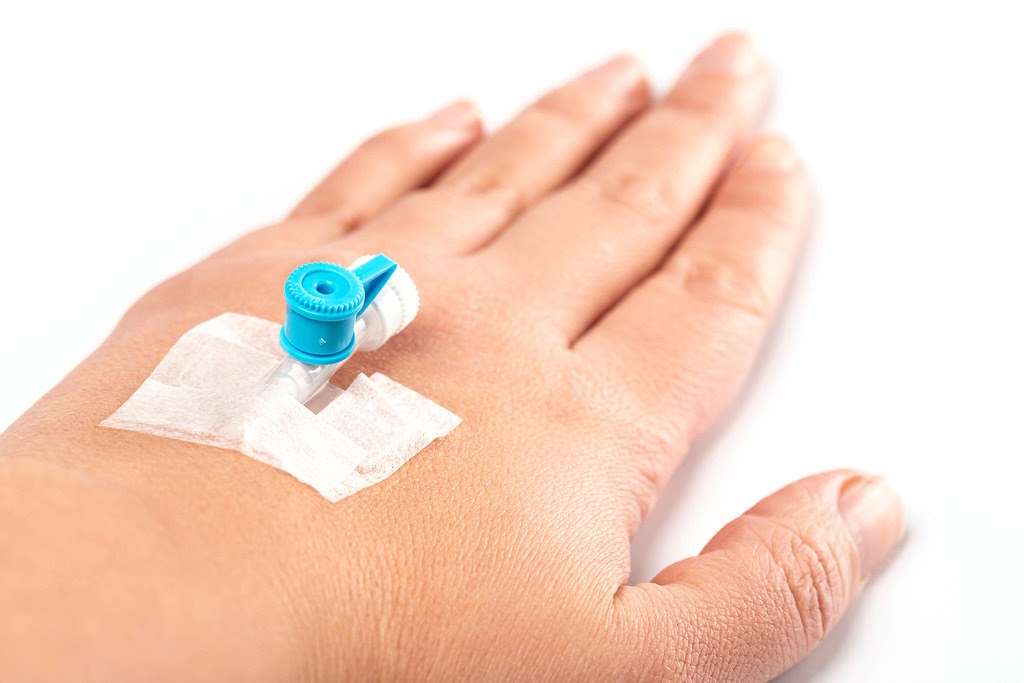
Before I go into the operating room, masked up with scrubs on, I see Mo again. It is easy to tell it is him; he’s a big guy. I am clenching my right fist, screwing my face up, preparing for the ‘scratch’ as the cannula gets introduced into a vein on the back of my left hand. It does not hurt. Mr Belci sticks his head in from the theatre room. I ask if I can keep the pump they’re going to remove? He replies jokingly to my request that he keeps all the old pumps to water his Orchids. I feel at ease as I am pumped with the anaesthetic and fall asleep – I always try to fight it, but it always gets the better of me!
I made it, I’m out of surgery
Bang! I am back. Nurses are sitting on either side of my bed. I need to drink and eat something. My mouth is dry, and a Digestive biscuit would be too gooey, so I go for the Fruit Shortcake with more gulps of water. During my time in Post Op, eating biscuits and drinking fresh water, the bed space opposite me gets vacated then filled pretty much immediately after by another patient. The nurse tells me the theatres are working at Max capacity for various ops. It feels like a massive production line to fix, repair and keep alive.
Heading back to my room on St Patrick’s ward, I see the anaesthetist team as I pass and thank them. Leaving the post-op recovery ward happy I have got through this procedure.
Back in my room, I realise I am hungry. More sandwiches! But better than nothing.
Nursing team
Being nursed by people younger than my spinal cord injury feels strange. I wonder if their training is as thorough as my years of experience living with SCI?
The nursing team is amiable, supportive, and don’t seem to mind me being chatty and asking questions. It is a multicultural team, and no one seems concerned about me asking questions about culture and why wet grey Aylesbury instead of sun and warmth. Housekeeping staff are on the ball as well. It must be a big operation to feed 24 beds every day – and that is just on this ward! There is a varied daily meal choice. I go for Chilli-Con-Cane for a couple of days, lentil cottage pie, but then venture for the curries. Sweet Potato & Lentil, then Chickpea Balti. None were quite the same as my local takeaway, and I think they all pretty much tasted the same! But it helped me pretend I wasn’t in the hospital.

Chickpea Balti meal choice is given as after surgery hospital meal. 
Sweet Potato Curry hospital meal choice
Due to regular bed changing, which ran in conjunction with bed baths, a large plastic bedding bag went to laundry services daily. Every occupied bed must go through this performance every day. That is a lot of bedding, washed, dried and ironed. The staff did not forget to throw the towels in as well. And a lot of towels were gone through during a wash!
The Surgeon visits
Mr Belci visits during his ward round the day after my surgery with an entourage of people. He shared operation details. Many medical terminologies were used to tell me what went on when I was out of it. I wasn’t sure what they meant. After asking questions, I got the gist that the procedure went well, the pump is in a slightly different position and is working fine, I will not get any withdrawal symptoms (thankfully!), I can go home a week on Friday. I will need to wear a brace, so I don’t lean forward, putting pressure on the scar by squeezing the pump between my thigh or lower rib. Being active, head chef at home, and generally getting on in life, this news is difficult to take in.
The working ward
I get disturbed from my slumber by the daily repetition of acknowledging that the housekeeping staff can enter my room, refresh water, empty bins, and order meals.

Constantly, Nursing staff get on with administering medication, taking Obs, washing, and generally making me feel comfortable and safe. BBC Six Music keeps me occupied, apart from Monday nights when my cousin is DJing on Stoke Mandeville Hospital Radio. A little TV helps fill some time between caregiver visits, but daytime TV seems to be all repeats – it must have been broadcast when I was last in, as I don’t watch daytime TV at home.
Mr Belci visited again on his ward round, and we discussed my discharge. He said I could transfer and carry on in life, do the school runs, cook and live. But I need to be careful; I have had major surgery on a repeated traumatised scar.
Preperation for home
It is the day before discharge. Karen, the physio for St Pats, is assisting me with transfers with the body brace on. She is on-hand for me to practice getting out of the bed into my wheelchair. I attempt these transfers after sitting upright for a few moments to let my head clear. Let the dizziness pass while my BP sorts itself out. Lying flat for ten days can do this.
Unfortunately, there is no time to attempt car transfers while an in-patient wearing this brace. I know each bed space is in demand, and if I don’t need to be using it, I might as well not be. There is also this thing going around called Coronavirus – I think I’m better out and recuperating at home. I get hospital transport to take me.
Transportation
The ramp into the back of the Ambulance looks steep. ‘I’m not going to be able to get myself up that‘, I tell the paramedic who is taking me home. I get pushed up, strapped in, and we head off.
A constant banging and rattling caused by every bump and pothole echoes in the space I’m sitting. Across the skinny aisle, sat next to the opposite window, is an elderly gentleman. Frank. He is not happy. From his complaints and discussion with the paramedics, I get the impression he is going to a care home, one he is not familiar with or where he wants to be.
I wish Frank all the best as the ambulance staff assists me out. Outside my home, my son is waiting for me. I smile, thanking the driver and wheel off. Climbing the ramp to my front door is a struggle. Do I lean forward that much while taking on a slope?
Announcement
Wheelchair skills training is on hold until early 2022.
Please get in touch with me if you would like to discuss training in the new year.
I’m sorry if this news disrupts any individual planes.
See you in 2022!
And lastly
A big thank you to the NHS. The National Spinal Injuries Centre staff at Stoke Mandeville, including the Nursing and housekeeping staff on St. Patricks Ward. The pre and post-op teams. Mr Belci, for his role in the procedure. Finally, everyone else associated with keeping the cogs turning for this national hero, to fix people, save lives, and make people as comfortable as they can. It’s a tough job!
The post Surgery – Theatre Day Arrives appeared first on Freedom Wheelchair Skills.